Is Lupus Genetic?Explore Lupus and what your DNA can tell you
What is lupus?
Lupus is a group of chronic autoimmune conditions that can affect many parts of the body, such as the joints, skin, lungs, kidneys, and heart. There are several types of lupus, but the most common type – called systemic lupus erythematosus (SLE) – can range from a small rash to severe disease that can affect multiple organs in the body. Symptoms and disease severity can vary widely from person to person and change over time, which can make recognizing and diagnosing lupus a challenge. Some common symptoms include fatigue, muscle and joint pain, fever, skin lesions, and a butterfly-shaped rash on the face. Although the cause of lupus is not fully understood, scientists think that the immune system becomes overly active due to a combination of genetics and environmental factors, resulting in damage to the body.
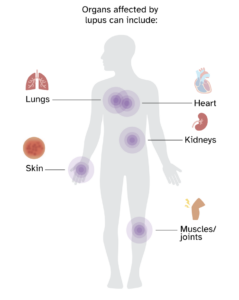
What can trigger lupus flares?
For people who have lupus, symptoms can come and go throughout life, but certain factors (called triggers) can increase the chances of flares. Some common triggers include:
- Sun or UV light exposure
- Certain medications (including certain antibiotics like sulfa-drugs or tetracycline)
- Illness or infection
- Injury
- Emotional or physical stress
- Exhaustion
Triggers and warning signs of a flare can vary from person to person. Learning personal triggers and warning signs can help to get treatment quickly and prevent severe flares. For people with lupus, it’s important to talk to a healthcare professional for help creating a management plan.

What are the health impacts of lupus?
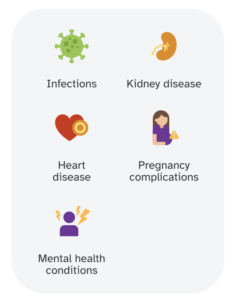
Lupus can increase the risk for many other health conditions, such as infections, kidney disease, heart disease, and pregnancy complications. But treatment for lupus can help manage these health impacts, in addition to reducing symptoms and flares. If you have concerns about lupus, talk to a healthcare professional. You may be referred to a specialist like a rheumatologist (a doctor who treats muscle-, joint-, and autoimmune-related conditions) or a dermatologist.
In addition, individuals with lupus may experience mental health conditions like anxiety and depression. Counseling and/or support groups can be an important part of some lupus management plans.
Is lupus genetic?
Genetics do play a role in lupus. This means some people may be more likely to develop lupus than others, depending on their genetics. Lupus can run in families, which means that a person has an increased chance of having lupus if family members have the condition. In fact, a four-year study by 23andMe and a collaborator of about 6,000 people with lupus found that about 28 percent of those who participated also had a parent, child, or sibling with lupus. In most cases, it is a combination of many different genetic variants that impact a person’s chances of developing lupus. Individually, each of these variants only has a small impact on a person’s genetic likelihood, but that impact can grow when many variants are considered together. 23andMe takes into account over 1,900 genetic markers to estimate the likelihood of developing lupus, but keep in mind that other factors besides genetics can also influence a person’s overall likelihood of developing lupus.
Other factors that may cause an increased likelihood of Lupus
Besides genetics, some factors that can increase a person’s chances of developing lupus include:
- Sex assigned at birth (about 9 out of 10 people with lupus are female, but lupus may be more severe in males)
- Ethnicity (lupus tends to be more common and severe from people of African, Asian, Hispanic/Latino, Indigenous American, and Pacific Island descent)
- Age (lupus is generally more common as people get older. For people who menstruate, lupus is often diagnosed prior to menopause.)
- Family history
- Currently taking certain medications (including some used to treat heart disease, thyroid disease, high blood pressure, and mental health conditions)
Find out if your genetics might increase your likelihood for developing Lupus
Curious whether you have an increased likelihood of developing lupus based on your genetics? Find out more with the Lupus report (Powered by 23andMe Research), part of the 23andMe+ Premium membership. 23andMe+ Premium includes our Health + Ancestry Service plus new premium reports and features throughout the year.

23andMe+ Premium
Please note:
- This report does not diagnose lupus and should not be used to make medical decisions.
- The report was developed by 23andMe scientists using data and insights gathered from thousands of customers who consent to participate in our research. Reports based on 23andMe research provide an estimate of your likelihood of developing a condition based on your genetics and other factors. This report does not account for lifestyle or family history.
- The report does not account for every possible genetic variant that could affect your likelihood of developing lupus.
References:
- Barber MRW et al. (2021). “Global epidemiology of systemic lupus erythematosus.” Nat Rev Rheumatol. 17(9):515-532.
- Centers for Disease Control and Prevention. “Managing Lupus.” Retrieved March 6, 2023, from https://www.cdc.gov/lupus/basics/managing.htm.
- Chen J et al. (2022). “Life factors acting on systemic lupus erythematosus.” Front Immunol. 13:986239.
- Fanouriakis A et al. (2021). “Update οn the diagnosis and management of systemic lupus erythematosus.” Ann Rheum Dis. 80(1):14-25.
- Fava A et al. (2019). “Systemic lupus erythematosus: Diagnosis and clinical management.” J Autoimmun. 96:1-13.
- Justiz Vaillant AA et al. (2023). “Systemic Lupus Erythematosus.” [Accessed Mar 6, 2023].
- Lupus Foundation of America. “National Resource Center on Lupus.” Retrieved March 6, 2023, from https://www.lupus.org/resources.
- Mayo Clinic. “Lupus.” Retrieved March 6, 2023, from https://www.mayoclinic.org/diseases-conditions/lupus/symptoms-causes/syc-20365789.
- Pons-Estel GJ et al. (2010). “Understanding the epidemiology and progression of systemic lupus erythematosus.” Semin Arthritis Rheum. 39(4):257-68.
- Stojan G et al. (2018). “Epidemiology of systemic lupus erythematosus: an update.” Curr Opin Rheumatol. 30(2):144-150.