Is Irritable Bowel Syndrome Genetic?Explore IBS and what your DNA can tell you
What is irritable bowel syndrome (IBS)?
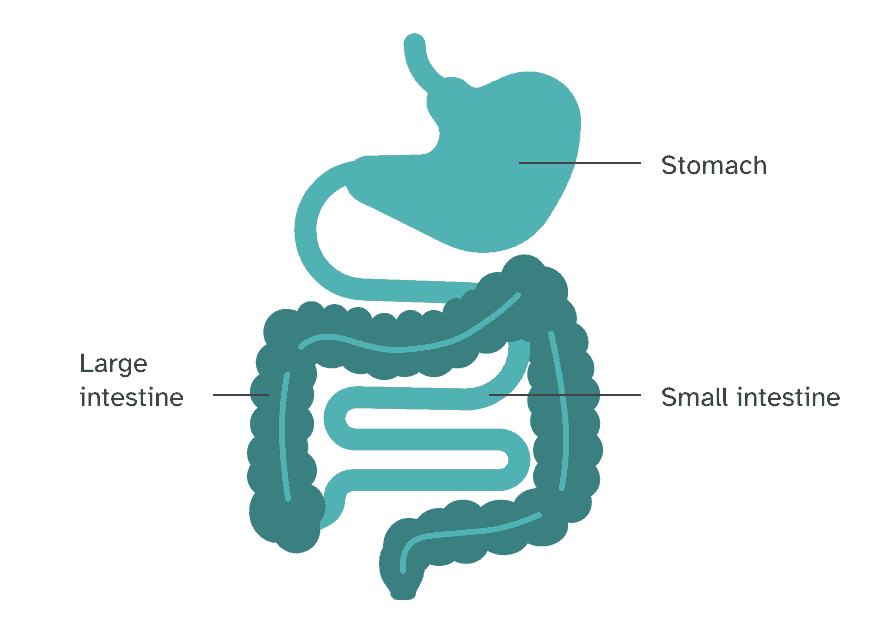
Irritable bowel syndrome, or IBS, is a disorder that impacts the large intestine. It causes symptoms like abdominal pain, cramping, bloating, gas, and changes in bowel movements, including diarrhea, constipation, or both. The cause of IBS is not well understood. Researchers think it may involve multiple related factors, including changes to how the brain and gut work together (called the gut-brain axis), changes in the makeup of microorganisms like bacteria that live in the gut (called the microbiome), and chronic, low-level inflammation in the intestines.
Find Out if Your Genetics Might Increase Your Likelihood for Developing IBS.
How can IBS impact your health?
The abdominal pain, diarrhea, constipation, and other symptoms that IBS causes can make day-to-day life a challenge. But IBS isn’t dangerous, and it doesn’t lead to increased risk of developing other problems with the intestines, like inflammatory bowel disease (IBD, a group of conditions that includes Crohn’s disease and ulcerative colitis). While IBS symptoms can come and go throughout life, there are many ways to manage them, such as identifying and avoiding symptom triggers. If lifestyle changes aren’t enough to control symptoms, medication may also be an option. Counseling may be helpful as well, especially if stress is a symptom trigger.
Is IBS genetic?
Genetics do play a role in IBS. This means some people will be more likely to develop it based on their genetics.
Find out how genetic testing for IBS works.
Did you know?
Studies suggest more than 10% of people have IBS. In addition to genetics, some factors that can increase a person’s chances of developing IBS include being younger than 50 years old, having a family history of IBS, being female, getting a severe digestive tract infection, or having a history of severe stress or abuse, including in early life.
Explore more
Interested in learning how your genetics may be related to irritable bowel syndrome? Find out more with the Irritable Bowel Syndrome report (Powered by 23andMe Research), part of the 23andMe+ Premium membership. 23andMe+ Premium includes everything in our Health + Ancestry Service plus new premium reports and features throughout the year.

23andMe+ Premium
Please note:
- The Irritable Bowel Syndrome report does not diagnose irritable bowel syndrome and should not be used to make medical decisions.
- The report was developed by 23andMe scientists using data and insights gathered from thousands of customers who consent to participate in our research. Reports based on 23andMe research provide an estimate of your likelihood of developing a condition based on your genetics and other factors. This report does not account for lifestyle or family history.
- The report does not account for every possible genetic variant that could affect your likelihood of developing irritable bowel syndrome.
References:
Chang L. (2011). “The role of stress on physiologic responses and clinical symptoms in irritable bowel syndrome.” Gastroenterology. 140(3):761-5.
Cleveland Clinic. “Irritable Bowel Syndrome (IBS).” Retrieved January 26, 2022, from https://my.clevelandclinic.org/health/diseases/4342-irritable-bowel-syndrome-ibs.
Cozma-Petrut A et al. (2017). “Diet in irritable bowel syndrome: What to recommend, not what to forbid to patients!” World J Gastroenterol. 23(21):3771-3783.
Johannesson E et al. (2011). “Physical activity improves symptoms in irritable bowel syndrome: a randomized controlled trial.” Am J Gastroenterol. 106(5):915-22.
Lovell RM et al. (2012). “Global prevalence of and risk factors for irritable bowel syndrome: a meta-analysis.” Clin Gastroenterol Hepatol. 10(7):712-721.
Mayo Clinic. “Irritable Bowel Syndrome.” Retrieved January 26, 2022, from https://www.mayoclinic.org/diseases-conditions/irritable-bowel-syndrome/symptoms-causes/syc-20360016.
National Institute of Diabetes and Digestive and Kidney Diseases. “Irritable Bowel Syndrome (IBS).” Retrieved January 26, 2022, from https://www.niddk.nih.gov/health-information/digestive-diseases/irritable-bowel-syndrome.
Ng QX et al. (2018). “The role of inflammation in irritable bowel syndrome (IBS).” J Inflamm Res. 11:345-349.